US diabetes patients face delays as insurers tighten Ozempic coverage
 Send a link to a friend
Send a link to a friend
 [December 12, 2023]
By Deena Beasley [December 12, 2023]
By Deena Beasley
(Reuters) - Some patients with type 2 diabetes say they are having more
difficulty getting reimbursed for drugs like Ozempic as U.S. insurers
implement restrictions designed to deter doctors from prescribing the
medication for weight loss.
Novo Nordisk confirmed in a recent email that it is seeing tighter
health plan management of GLP-1 drugs including Ozempic and is working
to minimize disruption for type 2 diabetes patients. The trend has
contributed to a recent dip in U.S. prescriptions, an executive at the
Danish drugmaker said at an investor conference last month. Out of 24
diabetes patients contacted by Reuters on Reddit, 13 reported recent
problems getting their health plans to cover Ozempic or Mounjaro, a
similar drug sold by Eli Lilly.
Elizabeth Beddow in Texas said her Blue Cross Blue Shield plan required
two other drugs be tried before it would pay for Mounjaro, which her
doctor prescribed after a diagnosis of type 2 diabetes. Instead, she was
prescribed Ozempic in March, which caused extreme fatigue and
gastrointestinal issues.
In September, Beddow, 57, was switched to an older drug, Lilly's
Trulicity, but said her blood sugar levels are still rising. Having to
start a low dose before moving up to a maximum dose with two different
medications was "really hard on my body," she said. "Ironically, my
insurance covers Mounjaro without step therapy on January 1." U.S.
regulators approved Ozempic for diabetes in 2017 and Mounjaro in 2022.
The drugs, more recently sold under the brand names Wegovy and Zepbound
for weight loss, are designed to mimic a hormone called GLP-1 to
regulate blood sugar, slow digestion and suppress appetite.

Most U.S. health plans cover GLP-1s for type 2 diabetes, which if
uncontrolled can lead to serious complications, including kidney failure
and limb amputations.
Sales of the self-injected medications, which have U.S. list prices of
over $1,000 a month, quickly soared into the billions, making the
companies among the world's most valuable. Sales have been limited in
large part only by manufacturing capacity.
"What's really resulted in kind of a more heightened focus on prior
authorization for the diabetes GLP-1 drugs is the increased volume from
off-label prescribing for weight loss," said Cory Midlam, director in
Willis Towers Watson's pharmacy practice, which advise employers on
benefits.
Health insurers Aetna, UnitedHealth and Cigna did not respond to
requests for comment.
PRIOR AUTHORIZATION ROADBLOCK
Some diabetes patients told Reuters that prior authorization, in which
doctors need insurer permission before prescribing a medicine, had
delayed by weeks, or even months, their ability to start a new
medication or stay on a drug they had been taking. Others said insurers
required them to try other drugs before their doctors were allowed to
prescribe a newer medication.
[to top of second column]
|
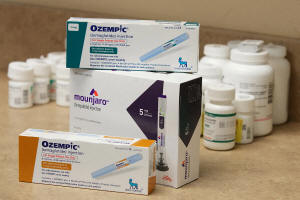
Boxes of Ozempic and Mounjaro, semaglutide and tirzepatide injection
drugs used for treating type 2 diabetes and made by Novo Nordisk and
Eli Lilly, is seen at a Rock Canyon Pharmacy in Provo, Utah, U.S.
March 29, 2023. REUTERS/George Frey/File Photo

A recent JP Morgan survey of U.S.
benefits executives found that 74% of large employer-based health
plans required diabetes patients to get prior authorization for a
GLP-1, and a third of the rest planned to add the requirement as
they grapple with higher spending on the medications as weight-loss
tools.
Doctors often have to provide evidence of diagnosis and document
that other medicines, such as generic metformin, were not adequate
to control blood sugar or caused intolerable side effects. The
average number of weekly Ozempic prescriptions rose 33% between the
first and third quarters of this year, but has since dropped more
than 6% to about 431,000, according to Iqvia Institute for Data
Science.
Doctors and patients are bracing for changes in January, when
individual health plans often set new coverage terms. "It may be
that January 1, all of a sudden something that was covered is no
longer," said Dr. Robert Gabbay, chief science officer at the
American Diabetes Association. Cost can also be an issue, especially
for patients who have high-deductible insurance plans. "Depending on
the coverage, some people still find it not affordable. That is
certainly a problem," Gabbay said.
Lilly, in an email, said it continues to help people with type 2
diabetes access Mounjaro, adding that some insurers may require
confirmation of diagnosis or prior diabetes medication use.
"You have to get prior authorization every year ... For us
physicians, a lot of our time is spent doing paperwork. It is
something that we all have to do, but it is a barrier," said Dr.
Anne Peters, an endocrinologist with Keck Medicine of USC in Los
Angeles. She said it is important that patients stay on a prescribed
treatment, and not get switched off a drug because of insurance
coverage. If the disease is controlled, she said, there is a better
chance of preventing things like heart disease, which is what
eventually kills most people diagnosed with diabetes.
"If it were an ideal world, you would use drugs like GLP-1s,
associated with weight loss, early," Peters said.
(Reporting By Deena Beasley; editing by Caroline Humer and Bill
Berkrot)
[© 2023 Thomson Reuters. All rights
reserved.]This material may not be published,
broadcast, rewritten or redistributed.
Thompson Reuters is solely responsible for this content.

|